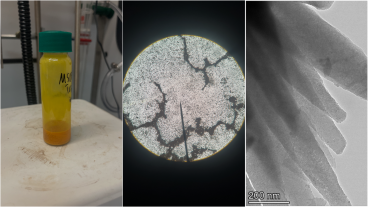
Drug-delivering microbots could help treat lacunar strokes
And not just any treatment — tiny bots that are designed to deliver a potentially life-saving medication straight to the problem area in the brain.
Strokes are the fifth leading cause of death in the United States, and a team of researchers at Colorado School of Mines is working on a new treatment for blockages that occur in vessels too small to be accessed by traditional catheters.
"If you have a stroke right now, there are two approaches to mitigating it. One is a catheter — you feed a catheter up there with the idea of physically removing the blockage. That works pretty well for larger vessels, the big ones in your brain where catheters actually fit. But about 20 percent of strokes are small-vessel strokes, lacunar strokes where catheters won't work," said David Marr, professor of chemical and biological engineering. "Another approach is using a clot-busting drug called tissue plasminogen activator, or tPA. tPA can also work, but it has a very limited therapeutic window— the drug has to be given to you intravenously within the first three hours of when the stroke begins or there are just too many complications."
Led by Marr and Keith Neeves, associate professor of chemical and biological engineering, the team has been awarded $2.6 million in funding from the National Institutes of Health's National Institute of Neurological Disorders and Stroke to further develop magnetically powered blood cell-sized microwheels, or microbots, capable of delivering tPA more quickly and directly to treat small-vessel strokes.
Specifically, researchers will use the funding to develop better ways to navigate the microbots through the body, determine and improve how quickly the bots can dissolve clots and determine just how much functional benefit they can provide in animals.
"The idea is microbot particles can be injected into the body, assembled in place with a magnetic field and then they're small enough to get to these small vessels where strokes occur but where catheters can't reach," Neeves said. "The big advantage is we can drive them to the point of blockage and then we can deliver the clot-busting drug on the particles. Instead of waiting for the drug to be diffused through the body, we can drive them to the site."
And once those microbots have completed their job, the magnetic field can be turned off and the bots will break down into individual particles again — another key advantage of the technology, Marr said.
"The particles are roughly the size of bacteria — white blood cells will recognize them and remove them from the body," he said. "Some other attempts to use small particles in the body, like nanoparticles, the problem is they are too small. They're too small for the immune system to recognize so they just stay there."
Earlier work by Marr and Neeves, funded by NIH, showed the feasibility of assembling and moving the microbots with magnetic fields in microfluidic models. The new funding will allow researchers to test the technology in physical models of increasing complexity and scale, starting with zebrafish larvae and moving to mice and life-size human replicas.
Also working on the project are Mechanical Engineering Assistant Professor Andrew Petruska and collaborators at University of Colorado Anschutz Medical Campus and University of Michigan.